NICE, the committee that sets NHS standards, has published a one-to-ten graduated scale for hospitals to use in deciding which Covid 19 sufferers to prioritise for ventilators, kidney dialysis and all the soon-to-be-rationed machinery of intensive care. Perhaps you have read the list and are thinking, “I’m fit, exercise regularly, have no other health conditions. I’m a One. If I get the virus the NHS will look after me. I’ll be fine.” They probably will but I promise you – you won’t be fine. Early this year I came down with double pneumonia, went into septic shock and almost died; the magnificent people of the NHS saved my life. In my disreputable youth I spent three months in the infamous Bangkok Hilton, Klong Prem Prison; in Jakarta I caught and survived a vicious tropical fever without medical attention. But my three weeks in ICU and the High Dependency unit at Southmead Hospital were still the worst days of my 71 years of life. Believe me – you don’t want to go there.
It happened so quickly. In the early hours of the 2nd of January I woke my partner. I was in bad shape – feverish, coughing, struggling with breathing. We debated whether to head for A&E in the morning or call for help now. Had it not been for our home blood pressure monitor I probably would have chosen to wait and would almost certainly have died. Fortunately, we strapped the cuff around my arm and received a terrible shock: 71/42 – about half what it should have been. I didn’t know it at the time but plummeting blood pressure is the septic shock signature tune. An hour later I was in the resuscitation unit at Southmead hospital, an x-ray showing both my lower lungs as a solid white mass. Double pneumonia had triggered sepsis and now I was in septic shock.
Very rapidly I went all the way to death’s wide open door – multiple organ failure, my body a war zone between impressively sophisticated medical science and aggressive, all-consuming infection exacerbated by the out-of-control guided missile that was my own immune system. Already by the following morning they had called in my partner to tell her to prepare for the worst. I was unconscious, of course. Not because of the disease but because they had knocked me out and pumped me full of muscle relaxants to keep me still. The things they have to do to you to keep you alive offer such brutal insults to your system you couldn’t bear it. You would thrash, groan, gibber, tear out tubes.
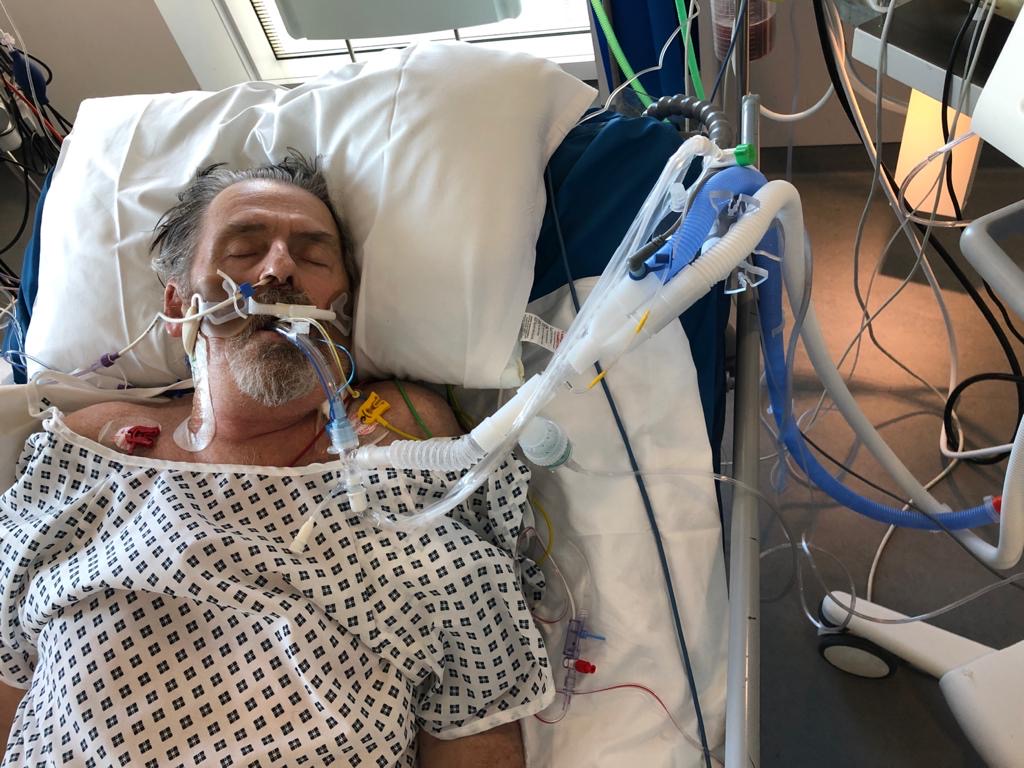
For me, those first six days of unconsciousness weren’t good, or bad, or anything. But for my family, my partner, they were hell. I could have died at any moment and the doctors could give no reassurances beyond promising to do their best. After the worst was over they slowly brought me back to some form of consciousness and now my nightmare started in earnest. My first clear memory is of the lovely face of my partner leaning over me. “Hello sweetie. You’re doing really well. Keep it up. You will be alright.”
Doing well at what, I wondered. Why could I not move? (Answer – muscle relaxants.) Why could I not talk? (Because of the tube down my throat, which I could not feel and did not know was there.) This was obviously a hospital. What had happened? Apparently I was told, more than once, but immediately forgot. I drifted off into the first of what was to be days of vivid, long-lasting hallucinations with complex, mad story-lines, all in other times and places, all extremely unpleasant. I was running some kind of bar in New Mexico or Arizona, desperate to get my hands on a cold, fizzy Coca-Cola or root beer which remained perpetually out of reach because, even in my hallucinations, I could not move.. I was bed-bound in a squalid inn in northern New Zealand sometime in the 19th century, waiting for my brother to arrive with bonds and deeds of title. Eventually he came, in a cocked hat and frock coat, but I could neither rise nor talk to him. I clearly remember six different such scenarios, all equally protracted and miserable. At unpredictable intervals I would be startled by a deafening beep, when the whole world would become a bright green undulating space of geodesic forms. Although they lasted only seconds such moments were almost indescribably terrifying, and they came often.
There were intermittent and fleeting moments of consciousness, usually the occasion of being rolled, shifted or washed, themselves mostly violent and shocking disturbances. Although I am sure they were being as gentle as possible the nurses had a non-stop workload to get through. There was never any time for me to prepare myself; just a brief warning and straight to it. I was aware of masked people flitting about in the half light. My first reaction was fear until I would get a grip on myself and remember that I was in hospital. Apparently it is not uncommon for intensive care patients to be seized by paranoia, to see witches and demons; at least I was spared that. Then there was the pain, misery and indignity of being dragged onto a coarse, compressed cardboard bedpan.
There is more – much more. As the hallucinations faded I became abusive, suspicious and resistant to help, demanding a saintly forbearance of staff and visitors. During the last days of those three weeks I was desperate, desperate to get out of that bed but when I tried I was told off in no gentle terms. Towards the end, when I was hoisted mechanically out of bed and into a special chair it was a triumph, surpassed only by the thrill of sitting on a real toilet. Those hideous, abrasive bedpans, how I hated them. After that I recovered very quickly, much faster than expected. Within a day or two I was walking with the aid of a stick and two days later I was home.
Why did I survive? Why, after predictions of long, slow months or even years of recuperation was I back to perfect fitness a scant six weeks after discharge? Simple. I don’t smoke, and for years now I have been walking a very brisk, demanding five miles on most days. I am very fit. I drove myself hard to get back into shape. Fitness has saved my life. But believe me, fit or not, you do not want a visit to ICU. Your loved ones and friends do not want you to be subject to the brutal mercies of ICU, nor do they want to spend days awaiting the news of your death. The health system certainly does not want you there. Bear in mind that I received the very best care the magnificent NHS had to offer. Now, we will get the best they can manage and it may not be enough.
I will go to any lengths not to catch this virus. I will willingly endure any inconvenience. And if you had been where I have been, so would you.
Thanks for this. I spent this morning scouring the Internet for descriptions of acute respiratory disease after a Guardian reader described it as like being waterboarded. Which oddly I found very helpful. As is your story. Just fix the typo in the first word of your title though!
LikeLike